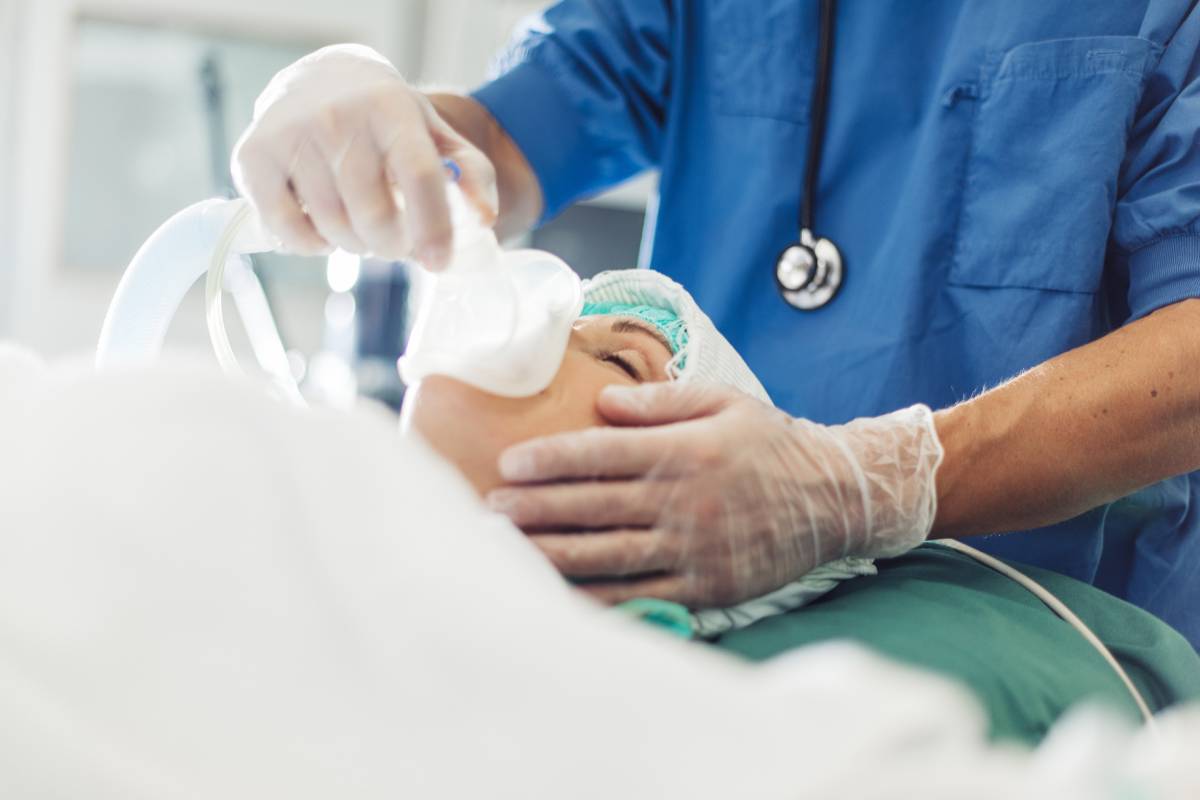
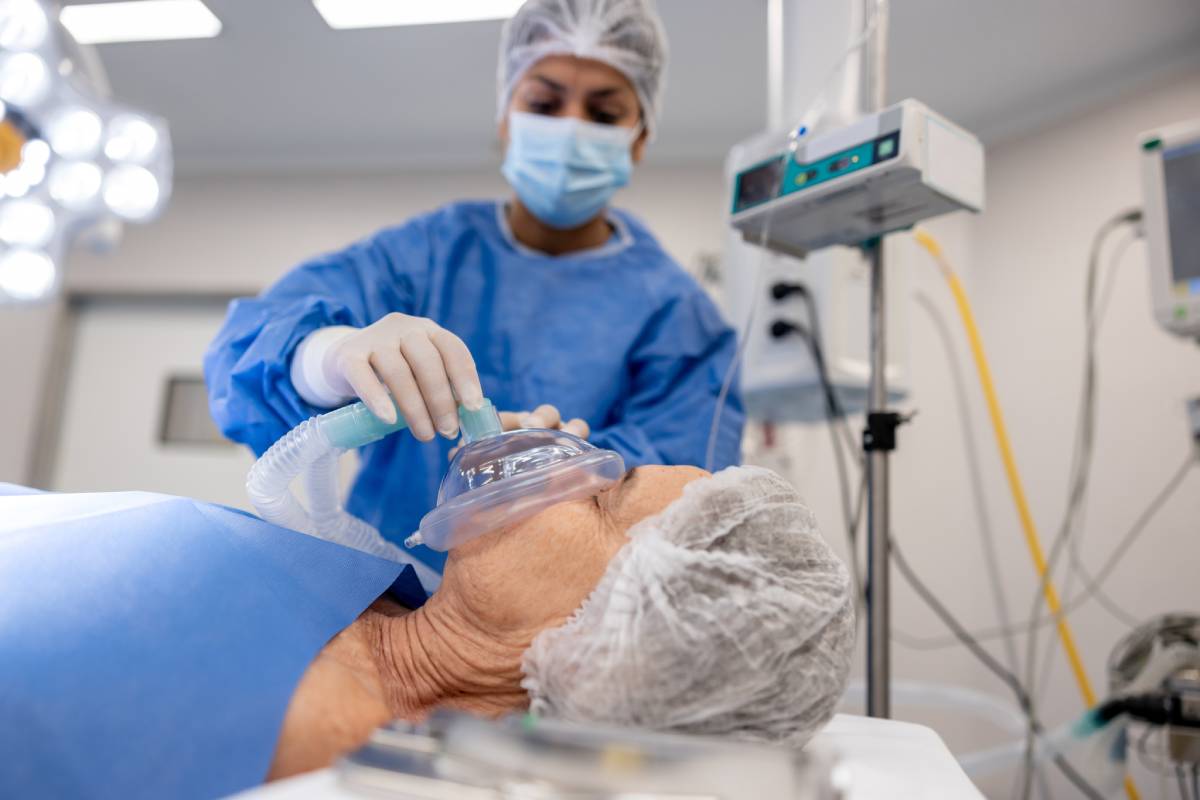
In otolaryngology, outpatient septoplasty is a common procedure indicated for symptomatic nasal septal deviation that contributes to obstruction, recurrent sinusitis, epistaxis, or impaired sleep quality. Advancements in surgical technique, anesthetic pharmacology, and perioperative monitoring have expanded anesthetic options for this procedure. One notable option is the use of moderate sedation in place of general anesthesia in selected patients. For anesthesia providers and ENT doctors, a careful comparison of moderate sedation against general anesthesia for outpatient septoplasty requires attention to patient safety, airway management, surgical conditions, efficiency, and postoperative recovery profiles.
General anesthesia has traditionally been the standard for septoplasty. It provides complete unconsciousness, airway control through endotracheal intubation or supraglottic devices, and immobility. These factors create optimal operating conditions, particularly in cases anticipated to be prolonged or technically challenging. A secured airway minimizes concerns about aspiration and facilitates controlled ventilation in the presence of intraoperative bleeding in or near the airway. General anesthesia may be particularly advantageous in patients with significant anxiety, low pain tolerance, or anticipated difficulty tolerating intranasal manipulation. Additionally, for combined procedures such as septoplasty with turbinate reduction or functional endoscopic sinus surgery, general anesthesia often offers superior conditions and procedural efficiency.
Moderate sedation, often combined with local anesthetic infiltration, represents an alternative for carefully selected patients undergoing isolated septoplasty. In this approach, patients maintain spontaneous ventilation and protective airway reflexes while achieving anxiolysis and analgesia. Sedative regimens may include benzodiazepines, opioids, propofol infusions at sub-anesthetic doses, dexmedetomidine, or a combination thereof. When administered by experienced anesthesia providers with appropriate monitoring, moderate sedation can provide adequate patient comfort while avoiding the physiological perturbations and slower recovery associated with general anesthesia.
Airway management is a central consideration in choosing between moderate sedation and general anesthesia, as septoplasty involves manipulation of the nasal passages and carries a risk of bleeding, which may track posteriorly. Under moderate sedation, the absence of a secured airway necessitates vigilant suctioning and positioning to reduce aspiration risk. Patients with obstructive sleep apnea, obesity, difficult airway anatomy, or gastroesophageal reflux disease are not ideal candidates for sedation-based approaches. In contrast, general anesthesia with endotracheal intubation provides definitive airway protection but introduces its own risks, including hemodynamic instability, airway trauma, postoperative nausea and vomiting, and delayed emergence.
Hemodynamic stability and perioperative stress response also differ between techniques. Moderate sedation, particularly with agents such as dexmedetomidine, may provide smoother hemodynamics and reduced sympathetic activation. Avoidance of positive-pressure ventilation may be advantageous in certain patients with cardiopulmonary comorbidities. Conversely, inadequate sedation can lead to patient movement, coughing, or hypertension, potentially compromising the surgical field. Close communication between surgeon and anesthesia provider is essential to titrate sedation depth while maintaining patient cooperation and safety.
Recovery profiles and resource utilization are increasingly relevant in ambulatory settings. Moderate sedation may facilitate faster recovery times, reduced incidence of postoperative nausea and vomiting, and earlier discharge readiness. Patients often experience less grogginess and may have a lower requirement for postoperative opioids when effective local anesthesia is used. From a systems perspective, sedation-based protocols may reduce anesthesia time and associated costs. However, these efficiencies must be balanced against the potential need for conversion to general anesthesia if patient tolerance proves inadequate.
Patient selection remains the critical determinant of success in sedation choice. Ideal candidates for moderate sedation are medically stable individuals undergoing isolated, straightforward septoplasty, who demonstrate the ability to cooperate and tolerate limited discomfort. Comprehensive preoperative evaluation should include assessment of airway risk, anxiety levels, comorbidities, and prior anesthetic history. Institutional capabilities, including immediate access to advanced airway equipment and skilled anesthesia personnel, are non-negotiable prerequisites.
Both moderate sedation and general anesthesia are viable options for outpatient septoplasty when applied judiciously. An individualized, multidisciplinary approach grounded in patient safety and procedural complexity should guide anesthetic choice in contemporary ambulatory otolaryngologic practice.